There are reproduction problems in 15% of married couples! Male factor in 1/3, female factor in 1/3 and both male and female factors in 1/3 of couples referred due to infertility are held responsible from the infertility. Therefore, there is a 50% of male factor in average.
Infertility may be defined as couples not achieving conception at the end of 1 year without applying any contraception method.
To start researchers with assessment of the MEN is cheaper, faster and easier.
A BRIEF OVERVIEW INTO THE REPRODUCTION PHYSIOLOGY
Human testicle is a double- functioned organ. In seminiferous ducts in the testicle; spermatogenesis occurs and Leydig cells within the interstitial tissue secrete steroid hormones (androgens). This is closely related with testicular functions. Testosterone (T) synthesis is not required for sperm production only, but also necessary for development of secondary sex characters and normal sexual activity. Gonadotrophins; LH (Luetinizating hormone) and FSh (Follicle stimulating hormone) are secreted from the frontal lobe of the pituitary gland on the brain. This activity is regulated by secretion of a hormone called GnRH (Gonadotrophin Releasing Hormone = Luteinizating hormone releasing hormone) by hypothalamus. Hypothalamo-hypophysieal gonadal axis continues on its function by a feedback control mechanism.
IN BRIEF:
THE REPRODUCTION SYSTEM OF A MEN MAINTAIN NORMAL ACTIVITIES BY OPERATION OF SOME CENTERS ON THE BRAIN AND TESTICLES AS A WHOLE WITH A REGULAR COOPERATION.
Main functions of androgens (MASCULINITY HORMONES) on the target tissue :
1) Regualtion of gonadotrophin secretion by hypothalamo hypophyseal axis (REGULAR OPERATION OF THE SYSTEMS ON THE BRAIN)
2) Initiation and maintenance of spermatogenesis
3) Differentiation of internal and external male genital system during intrauterine development of the fetus
4) Sexual development induction during puberty
Spermatogenez (sperm yapımı)
ermatogenesis
It is a complex process where spermatogonias have mitosis and produce into daughter cells by being transformed into spermatocytes. The most primitive forms of undifferentiated spermatogonias are root cells. Approximately 74 days are required for a whole spermatogenic cycle from primitive spermatogonium to development of a mature sperm.

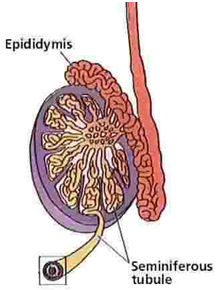
HORMONAL REGULATION OF SPERMATOGENESIS
Testosterone (T) production from Leydig cells within the testicle is stimulated by virtue of Luteinizing hormone (LH) which is produced in the brain and this affects the spermatogenesis indirectly. Seroli cells are target cells of FSH. T and FSH are hormones directed to seminiferous tubule epithelium.

SPERM TRANSMISSION, MATURATION AND STORAGE
Spermatozoa produced are immobile in the testicle and has no capacity to fertilize the ovum. Spermatozoa acquires the forward mobility and fertilization capacity after passing through the epididymis.
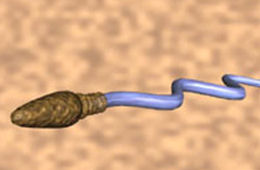

Sperms pass into a canal with a length of 5 to 6 meters called Epididymis. Epididymis consists of 3 sections as head, body and tail. Fertilization ability is completed on the cauda (tail) completely. Epididymis is also a reservoir for the sperm. Sperms deposited in the cauda of the apididymis enter into vas deference with a length of 30 to 35 cm which has a muscular nature and send the ingredient into the ejaculatory canal with peristaltic movements. Sperm is discharged with emission and ejaculation. Suring emission, secretions coming from the seminal vesicle and prostate are deposited in the posterior urethra.
First part of the ejaculate is rich in sperm and includes a little fluid. Most of the seminal plasma is provided from seminal vesicles (60%) and prostate (20%). Seminal fluid includes fructose, prostaglandins, phosphorylcholine and coagulating substances. Acidic vaginal media also buffers the seminal fluid. The coagulated semen (coagulum) created by the semen ejaculated liquefies with some enzymes secreted from the prostate within 20 minutes. All these steps are necessary for a normal fertilization.
FERTILIZATION
Normally, fertilization occurs in tubas (tubes in the woman) after the ovulation. Cervical mucus is more in the middle of the menstrual cycle, it starts to get thin and liquefy. These changes facilitate the sperm to enter into the uterus and move forward in the acidic vaginal environment. For the fertilization, spermatozoa should have physiological modifications in the female reproduction organ. Thus, sperm pierces outer layers of the oocyte and may create a whole by entering in.
ANAMNESIS (medical history)
It is very valuable. Presence of any previous contraception, presence of pregnancy of the previous or current partner should be evaluated. There are 4 main criteria for evaluation of male infertility: Anamnesis, Physical examination, Semen analysis (SPERMIOGRAM), Hormone analysis.
ANAMNESIS: HISTORY
Most men do not know when to have sexual intercourse for a pregnancy (80%). Use of lubricants during the intercourse affects sperm motility.
Previous fever, acute infections should be investigated so that these cause reduction in testicle functions and affect semen quality. In such case, the effect takes 2 to 3 months, because spermatogenesis is completed within 75 days. Furthermore, pelvic, retroperitoneal and bladder pathologies cause infertility. In these pathologies, retrograde ejaculation or unejaculation may occur ,n the reproductive system. Unejaculation or retrograde ejaculation occurs in those who has a testicle cancer and have been treated with retroperitoneal lymph node dissection due to effected sympathetic chain. This risk ratio has been reduced with new nerve protecting surgical techniques. Obstructions may be detected as a result of vas deference knotting mistakenly during hernia surgery. Patients who have undergone bladder neck resection may have retrograde ejaculation, therefore these type of operations should be investigated.
If mumps which is one of the pediatric diseases have occurred postpubertally, it is important. Infertility is met in 30% of the patients who had bilateral mumps orchitis after 11 years. Cryptorchidism (undescended testicle) should be asked as it will cause decrease on sperm production. Low sperm parameter is detected in 30% of the cases in unilateral cryptorchidism cases while this ratio is 50% in bilateral cases. 50% of the cases who have bilateral undescended testicle anamnesis are fertile. It should not be forgotten that, orchiopexy (descending the testicles) performed after first 2 years of the life will not increase the sperm quality or production.
Furthermore, reduction on sperm count of those working in pesticide production. A disruption on testosterone / estrogen hormone balance is in question here. Ionized radiation is also a risk and temporary reductions on sperm production may occur even with low doses such as 10 cGy. Sulphasalazine, cimetidine, calcium channel blockers, smoking, hashish use are gonadotoxic (toxic effect on sperm production) on testicles. Androgenic steroids preferred by people making body sport increase the muscular mass and play a contraceptive role related with fertility. Increased testosterone in the blood due to extra testosterone intake makes inhibition on hypophyseal gonadal hormone axis and almost stops sperm production in the testicles. If hot bath, steam bath is repeated routinely, the increase in intratesticular temperature spoils sperm production.
Cystic fibrosis should be asked in the familial background. This also progresses with intersex and congenital vas deference agenesis. Microdeletion of chromosome Y or karyotypic abnormalities should be investigated in the family. In case of any delay for the puberty, Kallmann or Kleinfelter syndromes should be considered.
ISSUES TO CARE ABOUT IN INFERTILITY ANAMNESIS
MEDICAL HISTORY
fever
Systemic diseases: DM – Ca – Infection
Genetic diseases: Cystic Fibrosis – Kleinfelter syndrome
Puberty initiation
SURGICAL HISTORY
Orchiopexy – cryptorchidism
Herniorraphy
Trauma – torsion
Pelvic – bladder or retroperitoneal surgery
TURP
FERTILITY HISTORY
Previous pregnancies (from the current partner or previous partners)
Infertility period
Previous infertility treatments
Evaluation of the sexual partner
SEXUAL HISTORY
Erection
Time and number of sexual intercourse
Lubricating use
FAMILY HOSTORY
Cryptorchidism
Kartagener syndrome
Hypospadias
Estrogen exposure
Prune Belly syndrome
MEDICATION HISTORY
Nitrofurantoin
Cimetidine
Spironolactone
Alpha- blockers
SOCIAL HISTORY
Alcohol
Tobacco
Cocaine
Anabolic steroids
HISTORY OF OCCUPATION AND ENVIRONMENTAL FACTORS
Radiation
Heat (setam bath)
Aniline paints
Pesticides
Heavy metals (lead)
PHYSICAL EXAMINATION
First of all, whole body should be assessed for hairing. Reduced body hair, gynecomastia, eunuchoid characteristic (length of the open arm is more than the body length)indicate androgen deficiency.
İnfertilite Sebepleri Scrotum should be palpated while the patient is standing. Two characteristics are noticeable here: Size and consistency of the testicles. Size may be assessed according to Prader Orchidometer. Standard testicle sizes are; average length is 4 cm, average width is 25 cm and average volume is 20 ml. Tight consistency is normal and soft consistency is abnormal. As 90% of size and consistency of the testicle is created by seminiferous tubules and germ cells, any mıdification may be considered as spoilt spermiogenesis. Also, irregularity and anterior location of the epididymis, induration, sensitivity and presence of cyst should be examined. Because 2% of infertile men has congenital vas deference deficiency, this should not be ignored during the examination. Enlarged pampiniform plexus makes the diagnosis of varicocele. Assymetry in the spermatic cord, sensing the venous dilatation when intraabdominal pressure is increased are assistant findings for the diagnosis. Varicocele is at the left side in general and left testicle is atrophic.
Furthermore, penile and prostatic pathologies should be noted. For example, hypospadias, abnormal curvature, phimosis. Temperature increase on the prostate and sensitivity during the rectal examination indicate prostatic infection. Enlarged seminal vesicle indicates obstruction of ejaculatory canal and this may be detected during the rectal examination.
LABORATORY
Urine Test:
It is a simple test that may be applied at office conditions. It shows infection, hematuria, glucosuria.
SEMEN ANALYSIS: SPERMIOGRAM
A careful semen analysis provides important information about male reproductive hormone cycle, spermatogenesis and solidity of the reproductive tract.
Abnormal semen analysis simply indicates decreased fertility. Normal semen quality has been reported by World Health organization (WHO) in 1992. Furthermore, spermiogram may also be assessed according to Kruger’s Strict Criteria. However, especially count and motility are the most important parameters for fertility.
- a) Semen Collection: Semen quality changes day by day and it is loosely associated with the collection technique. Sperm parameters widely varies according to the sexual abstinence. Semen volumei sperm consistency and total sperm count increase 0.4 ml, 10 to 15 million/ml and 50 to 90 million, respectively per each sexual abstinence day (until 1 week). If abstinence period is longer than 7 days, sperm motility decreases.
Therefore, the abstinence period suggested is 48 to 72 hours. At least 3 semen analysis should be performed to create a basis. Semen may be provided by masturbation, coitus interruptus ( this is suggested very rare) or into a wide-mouth condom including non-spermicidial agent, a clean glass or a plastic container. Because the sperm motility will decrease, semen should be analyzed within 1 hour.
- b) Characteristics and values: Fresh semen liquefies within 5 to 30 minutes. While coagulation factors are secreted from seminal vesicle, proteolytic factors (PSA) are originated from the prostate. Ejaculate volume should be 1.5 ml at least. Low volume ejaculate indicates retrograde ejaculation, ejaculatory duct obstruction, incomplete collection or androgen deficiency. Sperm concentration should be over 20 million at least. Sperm motility should be assessed within 1 to 2 hours. Normal motility is about 50 to 60%. It is classified from 0 ( no motility) to 4 (forward regular motility). Furthermore, sperm morphology and cytology are also determined. Head, body and tail parts of the sperm should evaluated. According to who, normal morphology should be 50% at least. According to Kruger’s classification, sperms below 4% is accepted as bad and above 14% is accepted as normal. Sperm morphology is associated with fertility potential.
- c) CASA: (Computer Aided Semen analysis): A computer assisted motility, morphology and concentration analysis is performed to resolve subjective changes of the manual analysis. Furthermore, nuclear characteristics of the sperm may be detected. Although this technique is promising, its possibility to provide sperm count over expected is 30% when leukocytes or immature cells are much. Also, high sperm concentration and motility may be lower than expected. CASA is a user- dependent technique and has an added value in the researches.
NORMAL VALUES IN SEMEN ANALYSIS
VOLUME: 1.5 – 5.5 ml
SPERM CONCENTRATION: <20 MILLION /ML
MOTILITY: >50%
FORWARD MOVEMENT: 2 AND ABOVE
MORPHOLOGY: > 50% WHO
KRUGER: >% 4
LEUKOCYTE < 1 MILLION /ML – Normal fructose content,
– No agglutination and leukocyte,
Explanation of defects in spermiogram:
* oligospermia: Sperm count below 20 million per ml.
* asthenospermia: Mobility under 50%
* teratospermia: Sperm deformity below 50%
* necrospermia: Dead sperms
* azoospermia: Not having any sperm in the semen
* aspermia: Complete lack of semen
SEMEN DEFECT RATIOS IN INFERTILE MEN
BEING EVERYTHING NORMAL: % 55
ISOLATED ABNORMALITY: % 37
Low motility: % 26
Low count: % 8
Low volume: % 2
Defective morphology: % 1
ASPERMIA: % 8
- d) seminal Fructose and Postejaculate Urine Analysis: Fructose is a carbohydrate derivation which is originated from seminal vesicle and present in normal semen. It is a kind of energy source, food of the sperm. In fructose absence, seminal vesicle aganesis or obstruction are considered. Presence of semen is searched in post-ejaculate urine test. If sperm is found, retrograde ejaculation should be suspected. It is especially necessary for patients with diabetes, pelvic, urinary bladder or retroperitoneal surgery. In some patients, orifice of the urinary bladder which should be closed is not closed while semen is excreted and some or all semen runs back to back (urinary bladder); therefore these patients may not have any sperm in the semen!!!
Hormonal Evaluation: Evaluation of Brain – Testicle (Hypophyso- gonadal) axis provides information about sperm production. FSH and testosterone level should be tested for pathologies occurred over hypophyseal axis (hyperprolactinemia, gonadotrophine deficiency, congenital adrenal hyperplasia) and patients who have sperm count below 10 million. Testosterone is the end product of hypophyseal axis and provides information about general endocrine balance of the reproductive system. If endocrine abnormality is present, serum LH and prolactin levels may be tested to detect the location of the pathology. Estradiol, Thyroid hormones, Liver tests may be ordered. Decrease on LH and FSH in normal spermatogenesis is not significant. Also, low LH and normal testosterone are not significant.
In brief; conditions that require hormonal assessment:
1) If sperm density is below 10 million /ml
2) If there is disrupted sexual function
3) If there are specific endocrinopathy findings (hormonal diseases)
ENDOCRINE PROFILE ON INFERTILE MEN
STATUS Testosterone FSH LH PRL
Normal male Normal Normal Normal Normal
Primary testicular failure Low High Normal/High Normal
Hypogonadootrophic hypogonadism Low Low Low Normal
Hyperprolactinemia Low Low/Normal Low High
Androgen resistance High High High Normal
SPECIFIC TESTS
Semen Leukocyte Analysis:
Semen Leukocyte Analysis:
Leukocytospermia or pyospermia = It is defined as presence of leukocyte over 1,000,000 in the ejaculate; it is the most important cause for sub-fertility. Pyospermia consists of 2.8% and 23% of infertile men. Neutrophils are seen most in leukocytospermia. Leukocytes look like immature sperms with a routine microscope, it is hard to differentiate. Therefore, they are called round cells. The stain used for differentiation is Papanikolau. Immature sperms and leukocytes are differentiated with this.
Antisperm Antibody Test (ASA):
Testicle is a strange organ and preferential immunologically. The reason for that is blood – testicle barrier. Autoimmune infertility occurs in case of damage in blood testicle barrier and exposure to sperm antigens. Sperm antigen secretion with an abnormal level occurs in 2 cases such as testicle trauma and vasectomy and this causes antisperm antibody (ASA) production. Disrupted sperm transport and disrupted ovum fertilization capacity are present in presence of ASA.
Criteria that will require ASA evaluation:
1) AGGLUTINATION in semen analysis
2) In anamnesis; testicle surgery or injury and low sperm motility
3) Increased round cell in the semen
4) Unexplained infertility
ASAs are present within 3 localizations. Serum, seminal plasma and sperm dependent. Antibodies are Ig M, Ig G and Ig A class. Ig A has a pure local origin. Immonubead Test (IBT) provides the most valuable information. Furthermore, there are Mixed antiglobulin reaction (MAR) and Radiolabeled antiglobulin test (RAT).
Hypoosmotic Swelling Test
Sperm Penetration Assay (SPA)
Sperm Cervical Mucus Interaction (PCT)
Chromosomal Studies
Genetic abnormalities may be present in male infertility. Azospermic (NONE SPERM AT ALL) or oligospermic (SPERM COUNT BELOW 20 MILLON/ml) infertile men may have abnormalities both on sex chromosomes and autosomes with a ratio of 2% to 15%. Blood test may be performed for cytogenetic analysis in presence of genetic abnormality. Patients with abnormal cytogenetic risk may have smaal atrophic testicles, high FSH levels and azospermia. Klinefelter syndrome (XXY) is a common abnormality in infertile men.
Cystic Fibrosis Mutation Test
This test should be applied to those with congenital bilateral vas deference agenesis and cystis fibrosis anamnesis. The Cystic Fibrosis gene is found in 80% of the men with a non-palpable vas deference. In the studies conducted recently, risk of Cystic Fibrosis gene is high in cases with sinusitis, bronchiectasis, obstructive azoospermia (Young Synd.) and in azoospermic cases who have idiopathic infertility.
Chromosome Y Microdeletion Analysis
One or more deletions are present in long arm of Chromosome Y in 7% of oligospermic men and 15% of azoospermic men with testicular failure. The most common microdeletion seen in infertile men is deletion of DAZ gene on AZFc region. None of the family members of these patients are fertile. Fertilization has been provided for these by using IVF and micromanipulation. For the people with small or atrophic testicles, for the identification of this dilation; blood should be taken in order to identify Y chromosome from peripheral locosite and also should be evaluated by polymerized chain reaction. (PCR)
Radiological Tests
Scrotal Color Doppler USG:
Scrotum evaluation may be performed by a high frequency (7.5 – 10 mHz) USG. Here, structure of the testicles is estimated and varicocele which is the most common cause for infertility and has the most successful treatment option may be detected. Diameter of pampiniform vein over 2 to 3 mm is abnormal. Also, presence of reflux flow is important.
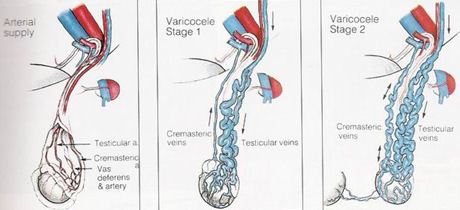
 Venography:
Venography:
It is the most definite diagnosis method known and gold standard for varicocele. While varicocele is detected in 30 to 40% of subfertile patients with palpation, this ratio increases up to 70% with venography. Because this test is expensive and technique dependent, it should be preferred to show relapses developed after the surgery.
TransRectal USG (TRUS):
Prostate, seminal vesicles and ejaculatory ducts are viewed by using high frequency 5-7 mHz USG. Stones, cysts and calcifications may be detected in dilated seminal vesicle (over 2.5 cm) and enlarged ejaculatory duct (over 2.3 mm) with TRUS. If low ejaculate volume accompanies to advanced oligospermic or azoospermic patients with decreased motility, TRUS should be applied.
Testicle biopsy and Vasography:
Testicle biopsy is used to establish the final diagnosis and to select the treatment in most infertility disorders. A small frame is opened onto the scrotal wall under local anesthesia and then tunica albuginea is opened and testicle tissue is removed.
Biopsy should be applied in azoospermic (none sperm in the semen) patients. It is difficult to differentiate the sperm production failure or obstruction in azoospermic cases. Biopsy provides important information about spermatogenesis.
Vazogram should be performed in cases whom obstruction is considered. Here, a contrast agent is administrated into vas deference. Proximal vaz , seminal vesicle and ejaculatory canal anatomy are determined by this way. Meanwhile, vasal fluid sampling and detection of sperm presence may also be done.
It is problematic to apply biopsy to oligospermic patients. Biopsy may be applied in case of obstruction, however its indication is less beyond this.
While unilateral biopsy is enough in general, bilateral biopsy is more assured. The condition for FSH level not being twice more than normal among biopsy indications was used to be sought in the past. However, it may be applied to patients with atrophic, insufficient testicle and high FSH level as well in terms of obtaining sperm that will be used for IVF and ICSI (assisted reproduction techniques). Because sperm has been detected in 30% of this type of patients.
Fine needle aspiration:
Although testicular sperm is sufficient to obtain pregnancy with IVF and ICSI, there is a failure to obtain sperm in 25 to 50% of the patients with advanced testicle insufficiency. Percutaneous fine needle aspiration has been defined to minimize failure chance for ontaining the sperm. With this technique, sperm is obtained in 60% of non- obstructive azoospermic patients and testicle mapping is performed. This technique is applied under local anesthesia in office environment. Seminiferous tubules aspirated are smeared, fixated and read by a cytologist and presence or absence of sperm is interpreted. This technique is a technique protecting the testicle rather than a biopsy.
Semen Culture:
When semen culture is applied to all infertile men, 83% provide positive result, therefore no cooperation has been established between infertility and semen culture.
Sperm culture is indicated is there is a suspicious case.
1) Anamnesis for genital infection
2) abnormal prostatic fluid secretion
3) Pathogenic bacteria more than 1,000 per milliliter of the semen
4) Leukocytes more than 1 million per milliliter of the semen
Gonorrhea is the most common infection. 10 to 25% of Klamidia infections progress asymptomatic. Trichomonas vaginalis, a protozoa parasite causes 1 to 5% of nongonococcal infections. Ureaplasma ueralyticum is the most frequent agent detected in urethra of sexaually active men and responsible from 25% of nongonococcal infections. Eschericia coli is rare in young males and a symptomatic infection in general.
MOST FREQUENT CAUSES FOR MALE GENITAL INFECTIONS
- Gonorrhea- Chlamdia Trachomatis – Trichomonas vaginalis – Ureoplasma urealyticum – Ech. Coli – Mycoplasma – Cytomegalovirus – Herpes Simplex II – Human papiloma virus – Hepatit B virus – HIV ( AIDS )
CAUSES FOR INFERTILITY (IN TITLES)
- PRE-TESTICULAR (cerebral causes):
HYPOTHALAMIC DISEASES
Gonadotrophin deficiency (Kallman syndrome)
Isolated LH deficiency (fertile eunuchoid)
Isolated FSH deficiency
Congenital hypogonadotrophic syndromes
HYPOPHYSEAL DISEASES
Hypophyseal failures
Tm – radiation – Infiltrative diseases – operations
Hyperprolactinemia
Exogen hormones
Testosterone – Estrogen – Cortisone – Thyroid hormones
Growth Hormone deficiency
Over operation of thyroid gland (hyperthyroidism)
Poor operation of thyroid gland (hypothyroidism)
- TESTICULAR
Chromosomal
Klinefelter syndrome XXY
XX sex reversal syndrome
XYY syndrome
Noonan Syndrome (male Turner syndrome)
Myotonic dystrophy
Vanishing testes syndrome (bilateral anorchidia)
Sertoli cell only syndrome (germ cell aplasia)
Micro deletion of chromosome Y
Gonadotoxins
Radiation
Drugs
Systemic diseases
Renal failure
Liver failure
Sickle cell anemia
Defective androgen activity
Testicle damage
Orchitis
Torsion
Trauma
Cryptoorchidism (undescended testes)
Varicocele
Idiopathic
- PORT TESTICULAR
Obstructions
Congenital
Vas agenesis
Young syndrome
Idiopathic epididymis obstruction
Polycystic kidney disease
Ejaculatory duct obstruction
Acquired
Vasectomy
Groin surgeries
Infection
Functional blockage
Sympathetic nerve destruction
Drugs
Sperm function and motility disorders
Immotile cilia syndrome
Maturation defects
Immunologic infertility
Infection
Coitus problems (related with sexual intercourse)
Impotence
Hypospadias
Timing and frequency
DRUGS DISRUPTING EJACULATION
Antihypertensives
Alpha adrenergic blockers
Thiazides
Antipsychotic agents (Tioridozin Hcl – Haloperidol – Chlordiazepoxide)
Antidepressants (Imipramine – Amitriptyline)





