UROLITHIASIS (URINARY SYSTEM STONES)
As clinicians, we interest in diagnosis and efficient treatment of the stone disease. However, medical treatment to decrease relapse of the stone formation and metabolic research that will provide lifestyle changes (evaluation) are as important as the stone treatment. 5 years stone relapse without any follow-up and medical treatment is about 50%.
The urine includes a liquid part and this liquid part includes some crystal and organic substances dissolved. When ratios of these crystal etc. substances within the urine increase (supersaturation), they loose their solubility and cause stone formation.
Supersaturation depends on urine pH, ionic strength, solute concentration and ability to make complex. Solubility of substances within the urine may vary dramatically in different physiological conditions. Such as urine becoming alkaline after meals while the first urine is relatively acidic in the morning.
MECHANISMS FOR STONE FORMATION

FREE PARTICLE THEORY :
It is not supported much. The crystal mass settles on the distal tube and collector tubes and grows.
FIXED PARTICLE THEORY :
Crystals adhere into the tube cells or into their walls and grows there until the stone forms.
THEORY OF AGENTS MODIFYING THE CRYSTAL FORMATION :
INHIBITORS :
They are agents that prevent stone formation in the urine.
Mg, citrate, pyrophosphate, acidic glycoprotein (nephrocalcin), alanine, Glycosaminoglycan (GAG)
COMPLEXORS :
They create more soluble compounds by binding with calcium (Ca) and prevent stone formation.
Phosphate, Citrate, Sulfate, Mg ( Mg and citrate are both inhibitors and complexors)
PROMOTERS Agents that trigger stone formation :
THM (Tamm – Horsfall Protein = Uromucoid = Matrix + 3% Cyalic acid), GAG (glycosaminoglycan), Matrix ( a kind of protein).
HOMOGENOUS NUCLEATION :
It is formation of a pure stone as a result of supersaturation of just one type crystal within the urine.
HETEROGENEOUS NUCLEATION :
They are stones created by precipitation of other types of crystals over the tissue, matrix, protein or other crystals. The supersaturation concentration required for heterogeneous nucleation is less than that required for homogeneous nucleation. (example: Calcium phosphate (CaPO4) and Uric acid stones may form a heterogeneous nucleation focus for Ca Oxalate stones).
NUCLEATION THEORY :
Nucleation theory suggests that urine stones are created by foreign bodies and crystals within the supersaturated urine. However, patients who discharge much urine or on dehydration do not always have stones. Furthermore, 24 hours urine and ion densities that create the stone are completely normal on those who have stones.
CRYSTAL INHIBITION THEORY :
It suggests that stone is created due to absence or low density of stone formation inhibitors such as magnesium (Mg), citrate, pyrophosphate, acidic glycoprotein (nephrocalcin), alanine, Glycosaminoglycan (GAG). As many people who do not have these inhibitors never have a stone and people who have these inhibitors much have stones inconsistently, this theory does not have any absolute validity.
URINARY IONS
- Calcium (Ca) :
It is the primary ion present in urinary crystals. More than 95% of the Ca filtered from kidneys is reabsorbed into the blood again. Less than 2% is discharged with the urine. Factors that provide Ca soluble are ability to create a complex with citrate, phosphate and sulfate. Increase on monosodium urates and decrease on urinary pH disrupts this complex creation ability and triggers crystal accumulation. More than 4 mg/kg/day Ca discharge within the urine ( 200 – 300 mg/day) means HYPERCALCIURIA.
- Oxalate :
10 to 15% passes into the urine from the food. Oxalate entering into the large intestine exposes to bacterial dissolution. The oxalate absorbed from the small intestine is not metabolized and discharged from proximal tubules. Presence of Ca within the intestinal lumen affects the absorbed oxalate quantity. Control of the oxalate within the urine plays an important role in creation of Ca- Oxalate. It may create a complex with Mg and Na within the urine. Normally 20 to 45 mgs of oxalate is discharged within the urine. Small changes on urinary oxalate level affects supersaturation of Ca-oxalate significantly. Principal precursors of the oxalate are glycine and ascorbic acid. Hypercalciuria may develop especially in inflammatory bowel disease, resection of small intestines. 5 to 10% of these patients develop kidney stones.
- Phosphate (PO4) :
Phosphate is an important buffer and creates a complex with urinary Ca. It is the key component of Calcium Phosphate (CaPO4) and Magnesium Ammonium Phosphate (MgNH4PO4) stones. Urinary phosphate excretion on normal adults depends on the phosphate quantity within the diet (meat, milk, vegetable). The PO4 filtered from glomerulus is reabsorbed from the proximal tubule. A hormone (PTH) secreted from the parathyroid gland inhibits this absorption. Therefore, patients with hyperparathyroidism have stones frequently. Normally, 500 to 1100 mg/day phosphate is excreted by the urine.
- Uric Acid :
Uric acid is a side product of a specific protein (purine) metabolism. Uric acid quantity increases below pH 5.5. 10% of the filtered uric acid passes through the urine. Defects on purine metabolism may cause uric acid stone formation. Pure uric acid crystals and stones are non-radiopaque and may not be seen on direct urinary system radiographs (DUSR). Some uric acid stones may be radiopaque because of Ca accumulation. It should be excreted less than 800 mg/day in normal.
- Sodium (Na) :
Although Na is not one of main components of most of urinary tract stones, it plays an important role in Ca crystallization. Na triggers crystal development and aggregation. Na reduces Ca reabsorption from proximal and distal tubulus. High Na intake (table salt) with the diet increases Ca excretion within the urine, reduces urinary pH and citrate excretion. Thus, ability of the urine to inhibit Ca oxalate crystal aggregation is corrupted. On the contrary, reduction of Na in the diet causes reduction of nephrolithiasis (stone) cases.
- Citrate :
It is the most important inhibitor agent. Normally, 450 to 800 mg is excreted by the urine per day. Excretion less than 400 mg/day is a risk for urolithiasis. = HYPOCITRATURIAIf intracellular metabolic acidosis develops by any cause 8hypopotasemia – Hypomagnesemia – hunger – acidic diet – Chronic diarrhea), the citrate deficiency that will arise frequently causes stone formation. Androgens decrease the citrate. Estrogen accelerates citrate excretion and reduces stone formation in women during pregnancy.
- Magnesium (Mg) :
Mg deficiency within the diet is together with increased urinary tract stone incidence. Mg is present within the compound of struvite stones. Empirically, Mg deficiency within the diet is associated with increase on Ca-oxaşate stone formation and Ca-oxalate crystallization. Mechanism of action of Mg is knot known clearly and Mg supplementation done to normal individuals does not protect them against the stone. Daily Mg excretion should be over 60 mEq.
STONE TYPES
ACCORDING TO THEIR CHEMICAL STRUCTURE

Ca-Oxalate (monohydrate = whewellite hard stone, dehydrate = weddellite soft stone; stones that are effected by pH)
Ca-Phosphate (it is the hardest stone; hydroxyapatite, carbonate apatite, amorphous calcium phosphate = brushite; it tends to precipitate in alkaline pH)
Struvite (Mg- Ammonium- Phosphate; it precipitates on alkaline pH)
Uric acid (it precipitates on acidic pH)
Cystine (it precipitates on acidic pH)
Xantin (it precipitates on acidic pH)
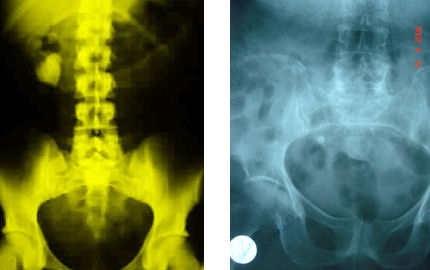
STONES ACCORDING TO THEIR RADIOPACITIES (visibility on direct gradiograph)

Ca-Pfosphate – Ca-oxalate – Struvite (radiopaque)
Cystine (semiopaque)
Uric acid – xantin (non-opaque)
CALCIUM STONES
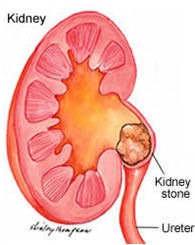
Nephrolithiasis (kidney stone) appears after Ca settlement (calcification formation and accumulation) on collector system of the kidney. It includes 80 to 85% of all urinary tract stones. Ca stones depend on Ca increase, urinary uric acid increase, urinary oxalate increase and urinary citrate decrease.
When Ca- Na- Protein- Sulfate – Carbohydrate – Refined sugar increase within the diet or Phosphor decreases: Urinary Ca INCREASES.
In the diet; when phosphate – fibrous foods (Phytate and Fibers) increase, urinary Ca DECREASES.
DRUGS : While some drugs increase urinary Ca excretion and cause stone formation, some drugs reduce urinary Ca excretion and prevent stone formation.
Thiazides (drug reducing the blood pressure): They increase tubular reabsorption and reduce urinary Ca.
Loop Diuretics (drugs reducing the blood pressure): They reduce tubular reabsorption and increase urinary Ca.
Cellulose Phosphate: It binds the intestinal Ca and reduces its absorption; low Na diets and low oxalate diets should be recommended. It reduces urinary Ca and Mg. Mg supplementation is useful. They also increase effect of thiazides.
Alkalizing agents: Citrate salts: Recover metabolic acidosis and reduces urinary Ca.

STONES THAT DO NOT INCLUDE CA
Struvite :

Struvite stones consist of MgNH4PO4. It appears in women mostly and relapses rapidly. They are presented in the shape of renal stag horn calculus in general and they create urethral stone rarely.
Struvite stones is created by organisms that break down the urea (( proteus, pseudomanas, providencia , klebsialla, staphylococcus, mycoplasma). Organisms that break down the urea causes high NH4 concentration and alkaline urinary pH (<7).
Uric Acid :
All uric acid stones include less than 5% of all urinary calculus and incidence of the uric acid stone is high in gout, myeloproliferative disease, rapid weight loss, malign cases treated by cytotoxic drugs especially in men. Most of those with uric acid stone do not have hyperuricemia. Elevation of uric acid levels generally depends on dehydration and excessive purine intake. There is not any known inhibitor of uric acid stones.
Treatment is arranged to keep the urine volume > 2lt/day and urinary pH > 6. Purine decrease within the diet and allopurinol treatment reduces uric acid excretion. Alkalizing provides dissolution of Potassium citrate calculus and is dependent on the surface area of the stone. Surface of the stone fragments increases after the lithotripsy and they dissolve faster.
pH should increase to 7 at most in the treatment, if pH increases more CaPO4 stone formation risk begins!!!
If uricosuric drugs are given only for the treatment of patients with GOUT and urine is not alkalinized, uric acid formation increases; attention!!!
FINDINGS AND SYMPTOMS OF URINARY TRACT STONES
A – PAIN
The stone pain of kidney and urinary tracts are called renal colic. Colic pains are characterized with severe pain which decreases after a while and repeats again. The cause of the pain occurred here is that when the urine can not be discharged by the kidney which runs against the stone obstacle, it accumulates and this causes inflation of the kidney. Namely, pain of kidney stones means inflated, taut kidney. (Pain of the patients with renal calculus depends on the urinary obstruction).
Severity and localization of the pain depends on the size, location, obstruction grade, individual anatomical differences (extrarenal – intrarenal pelvis i.e.). Size of the stone does no correlate with severity of the symptoms. Pain frequently starts suddenly, it is severe and the patient takes different postures to reduce the pain.
RENAL COLIC – ACCORDING TO THE STONE LOCATION
- Kidney calyx :
They are small stones in general and tend to pass spontaneously.
- Kidney Pelvis :
As renal pelvis tones larger than 1 cm will cause obstruction on passage to the ureter, they create severe pain. The pain diffuses into the flank area (CVA – Costa Vertebral Angle) and upper abdomen on the same side (abdomen).
- Upper and Mid Ureter :
Upper and mid ureter stones cause severe and sharp pain on CVA and flank area. If the stone move down from the ureter and cause intermittent obstruction, the pain is severer and intermittent. If the stone has stuck in a place and cause partial obstruction, it may cause less pain. Upper ureter stones cause pain on lumbar region and flank while mid ureter stones cause pain on middle and lower section of the abdomen.
- Distal Ureter :
Lower ureter stones cause a referred pain on the testicles and the groin in men and labia majora in women.
- Intraluminal (ureter part extending within the bladder) : Ureter stones may cause some cystism symptoms such as cystitis, prostatitis, pain on the penis tip, frequency, urgency, dysuria, strangury or gross hematuria and imitate diseases of these organs.
B- HEMATURIA (bloody urination)
In general, patients refer if there is an intermittent gross hematuria accompanied to the pain or tea colored urine (old hematuria) are present. Most patients develop microscopic hematuria at least.
C- INFECTION
MgNH4PO4 stones mean infection stones. It is together with proteus, pseudomonas, providencia, kelbsiella and staphylococcus infections. All stones may be together with an infection secondary to the obstruction and stasis. Specific antibiotics against the germ in the urine culture should be given before elective procedures.
ASSESSMENT
- Differential Diagnosis
A differential diagnosis should be done for emergency cases called acute abdomen such as acute appendicitis, ectopic pregnancy, pathologies of the ovaries, diverticular diseases on intestines, intestinal obstructions, gall bladder stone, peptic ulcer, embolism of the acute renal artery, abdominal aorta aneurysm. Peritoneal findings should be assesses by a medical examination.
- Medical Story
Initiation, character, dissemination of the pain; activities that increase and decrease the pain; accompanying nausea and vomiting and similar pain history should be investigated. Those who have stone previously have a pain history similarly.
- Risk Factors
- Crystals :
Those who develop stones, Ca oxalate stones in particular excrete more Ca oxalate crystal within the urine and these crystals are larger than normal. Stone formation ratio is proportionate to the percentage of large crystals and crystal aggregates. Urine samples should be fresh, be centrifuged and examined immediately. Presence of cystine and struvite crystals within the urine is abnormal and requires further investigation. Other crystals are present in the normal urine analysis.
- Socioeconomic Factors :
Renal stone disease is more common in industrialized countries.
- Diet :
Saturated, insaturated fat acids, animal originated proteins increased fiber, vegetable protein and unrefined carbonhydrate may decrease stone incidance.
- Occupation :
Incidence increases for those who work under high temperatures which may cause dehydration and in jobs with less physical activity.
- Climate :
Hot climate may cause dehydration which increases uric acid stone incidence in particular. Hot climate also causes to be exposed to ultraviolet light more and Vitamin D3 increase. This increases Ca absorption from the intestines.
- Family Background :
Those who have stone history in their family have a high incidence of urinary stone. Incidence is 2 times more in the patients with family history than those without family history.
- Drug :
Stone formation possibility increases for those who use antihypertensive (triamterene), antacids (including silica), carbonic anhydrase inhibitors.
Physical Exmination :
Pain is severe in renal colic and the patient tries to reduce the pain by changing her/his posture. Systemic findings are tachycardia, sweating and nausea. Severe pin occurs in the examination performed in the form of impact onto the lumbar region.
In complete urine analysis;
Macroscopic (visual) or microscopic hematuria (bleeding), leukocyte increase which is a finding for infection and crystals that is called sand in the public may be detected.
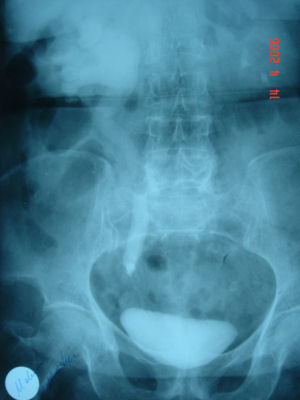
Radiology :
For every patient referred for stone or similar complaints, direct urinary system radiography (DUS) should be taken after the urine test and a complete abdominal ultrasonography (US) should be applied by considering the differential diagnosis.
As we specified above, 85% of the stones include Ca, therefore they may be seen in direct radiographies. US should also be taken to see whether a dilatation is present in the kidney.
If a final diagnosis can not be established by these two tests; Uropgraphy (IVP) taken by administrating colored agents intravenously or Computed Tomography (CT) with or without intravenous colored agent may be utilized.
TREATMENT
OBSERVATION AND ASSISTANT AGENTS
Most ureter stones pass spontaneously and no intervention is required.
Spontaneous passing depends on the size, shape, location of the stone and accompanying ureter edema.
Possibility of passing an ureter stone with a size of 4 to 5 mm spontaneously is 40 to 50%. Spontaneous passing possibility of the stone larger than 6 mm is less than 5%.
Most of the stones passed passes within 6 weeks after initiation of the symptoms.
The possibility of distal ureter stones and proximal ureter stones when symptoms appear is 50% and 5 to 10%, respectively.
At this observation stage, patients are required to move a lot and drink much water (3 liters fluid at least per day)!!!
If pain occurs at this stage, hot application is very useful. Putting hot water into the plastic bags called thermophore and applying onto the aching area rapidly recovers the pain or filling the bath tub with hot water and sitting in it will also be useful. “Drinking bear” which is told within the public has no additional benefit. The main purpose is to intake fluid much and to urinate much and facilitate movement of the stone.
OBSTRUCTION DISAPPEARANCE
Urinary stone disease may cause significant morbidities and early mortality with presence of the obstruction. If fever and infected urine is present in the patient with obstructive urinary stone, urgent drainage (providing the urine flow) is necessary.
Stone diseases are those where endo-urology is used most. Here, various diagnosis and treatment alternatives may be utilized by using camera optic systems without necessity of open surgical interventions. When obstruction is present, retrograde pyelography which is applied to define the upper urinary system when necessary is followed by retrograde Double – J stent placement. This is the most efficient technique to resolve the obstruction.
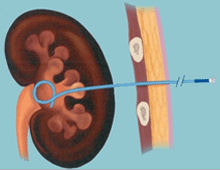
If this method can not be achieved (when the stone can not passed blindly or by seeing with tools inserted from the external urinary tract), kidney is accessed by percutaneous nephrostomy (by opening a hole from the back) and a tube is placed into the kidney and urine flow is provided.
ESWL (Extra corporeal shock wave lithotripsy) STONE BREAKING SYSTEM OUT OF THE BODY


ESWL has been found in Germany in 1980s and marked a new epoch for the stone treatment. The purpose of the treatment is that focused shock waves pass through the body and breaks the stone into fragments when such waves come onto the stone. These shock waves may be created by using different technologies (spark gap-piezoelectric crystals – electromagnetic energy). First generation machines were used to require a large place and general anesthesia were used to require for the procedure and patients were used to lie within a system filled with water. Shock waves pass thorough water and soft tissue with minimal energy loss and less injury, they create a mechanical effect on the targeted material. It causes the stone to be dilated and separated into small fragments.
The 3rd generation machines which are used today has been converted into quite small and compact pattern. Furthermore, neither a water pool nor anesthesia are required. 1000 to 4000 shock wave shoots are done per session which lasts thirty minutes in average and most of the patients do not FEEL PAIN. Some patients may have pain due to the sensitivity or size or location during the stone breaking procedure; even for such cases, it is not necessary to anesthetize or narcotize. Intramuscular analgesic application will be sufficient and breaking procedure may be applied.
The patient is awake during the stone breaking procedure and she/he may talk to the people around. Because stone breaking procedure may be applied in the office or polyclinic environment, it does not cause any labor power loss. The patient will be able to get up and get dressed at the end of the breaking procedure and continue on her/his work. The physician recommends her/his patient to drink water much and to move a lot after the first breaking session. Then, the patient is asked to come to the control visit after 3 days to 1 week. The patient is told to observe while she/he is urinating and that she/he may pass some particles like sand. Having pain during this period is quite natural. When severe pain occurs, local hot water application (thermophore) or sitting in a bath tub filled with hot water will relax the patients. If pain is not resolved, analgesic injection or suppository is done under the control of the physician.
As ESWL may be applied solely for treatment of urinary tract stones, it established one part of double and triple therapies called combined therapy. Size, location of the stone and anatomical nature of urinary tract of the patient are very important here.
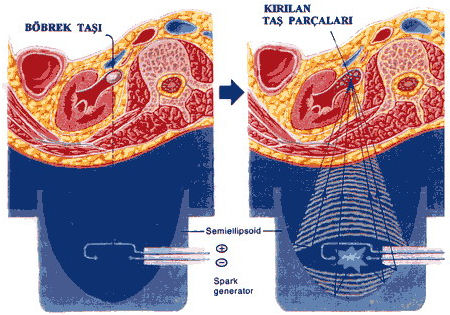
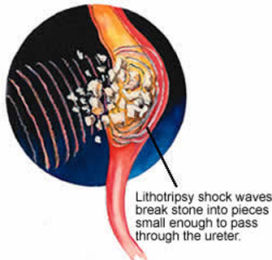
For example, ESWL may not be enough to eliminate the stone completely for kidney stones larger than 2 cm. In this case, it should be applied with Percutaneous nephrolithotripsy (PCNL). Sometimes, a stent (double-J stent) is placed into the kidney of the patient previously via cystoscopy to prevent aggregations of the stone particles (stone street) in the ureter. The advantage of this stent is to prevent the obstruction that may appear while breaking the stone in the kidney and severe pains that may appear by kidney dilatation due to this.

ESWL does not have complication much if applied regularly. It may cause bleeding in the kidney, flushing, hypertension crisis rarely. Kidney function changes that appear within the short period are completely temporary. It does not cause any permanent kidney damage. It is a safe technique. It should not be applied for pregnant women.
ENDOSCOPIC (CLOSED) THERAPIES They are benchmarks of the stone treatment.
– percutaneous nephrolithotomy- lithotripsy (breaking and removing the kidney stone with a closed system)
– Ureteroscopic lithotripsy (breaking and removing the ureter stone with a closed system)
– Cystolapaxy (breaking and removing the ureter stone with a closed system)
The purpose of all endoscopic systems is to approach the patient within a minimally invasive form and to handle the problem as simplest as possible. Whatever the insertion path is (by a small skin incision from the ilium for the kidney or outer foramen of the urinary tract for the bladder and ureter), breaking energies used are the same (ultrasonic- electrohydraulic- pneumatic- laser) and tools are also similar endoscopes with different sizes (cystoscope- ureteroscope- nephroscope).
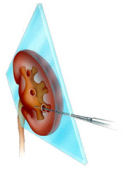
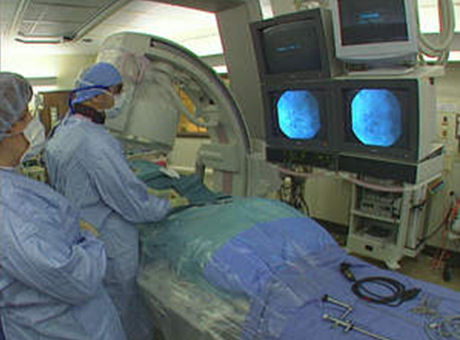
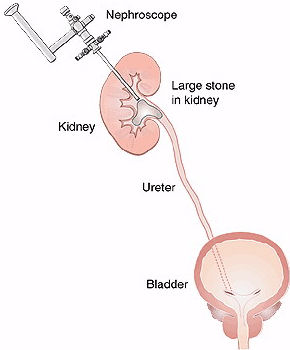
PERCUTANEOUS NEPHROLITHOTRIPSY (PNL)
After the patient is narcotized in the OR and the kidney system is entered via a needle inserted from the skin on the iliac area, a guide wire is placed into the system through this needle. The needle is removed and a balloon which is placed via this guide wire and may be blown is blown up to create a hole with an approximate diameter of 1 cm. An endoscopy tool called nephroscope is inserted into the system which was placed into the kidney over this balloon via a tube with an approximate diameter of 1cm and inner structure of the kidney is observed visually over the optic or by reflecting such image onto the monitors. In the meanwhile, information about location of the stones within the kidney is obtained. Then, a wire (probe) used for stone breaking is sent through the nephorscope and the energy whichever will be used is used and stone is started to be broken into small pieces slowly. The stone particles which become smaller meantime is removed in particles through the tube. A small tube (nephrostomy catheter) is placed into the system to stay for a temporary period ( 1 to 2 days) to keep the urine flow and rapid recovery after the procedure. This method provides an efficient and safe treatment option as a less damaging technique for removal of kidney stones(s). It is a minimally invasive procedure that requires a hospitalization period for 1 to 2 days in general.
Today, the first choice for large stones bigger than 2 cm and/or settled on the lower part of the kidney and for stenosis on uretteropelvic junction which is the corner where the kidney and ureter have joined should be PCNLa
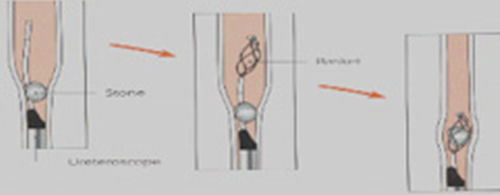
URETERORENOSCOPIC LITHOTRIPSY
The device used may be hard or soft. The purpose is the same. Bladder is entered first and then the ureter which includes the stone is entered through the kidney. There are uterescopes with different diameters and lengths in this procedure. Entering into the ureter may be done with different techniques. First, entrance aperture may be dilated with a balloon or ureter is entered via thin tools without necessity of doing this and stone is accessed. If the stone is small and the physician is experienced, the stone may be removed as is with a tool like hook called basket catheter or stone breaking probes are inserted into the tool and the stone is broken into small pieces by using any energy. After this step, stone particles are either left to pass spontaneously or removed by the basket catheter. This procedure is minimally invasive and may be applied as out patient in the hospital. The most important disadvantage is requirement of OR and narcotizing. However, it is the most successful method for ureter stones (distal ureter stones) within the osseous pelvis because the success of ESWL is lower due to the imaging difficulty.



CYSTOLAPAXY
It is the easiest method that may be applied to break bladder stones with a closed system beyond ESWL therapy. The bladder is entered via a classical cystoscope and the stone is broken either with mechanical tools and particles are removed via a pendant switch or stone breaking probe is inserted and the stone is broken into small pieces by using energy and removed via the pendant switch. It is an output procedure. It requires hospital and anesthesia, but it does not require hospitalization. The advantage is that if there is any other pathology of the bladder neck or urethra, it may also be treated within the same session.
OPEN SURGICAL THERAPY

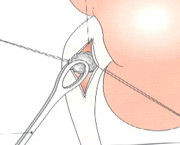

Main open surgery methods are;
Pyelolithotomy (removal of kidney stones from pelvis renalis),
Nephrolithotomy (removal of kidney stones by opening the kidney parenchyma),
PROPHYLAXIS
Those who do not care about prophylaxis methods have relapse (stone formation again) with 50% within 5 years.
TRUTHS ON PROPHYLACTIC TREATMENT
* THE PATIENT SHOULD DRINK 2 LT. FLUID PER DAY.
* THE PATIENT SHOULD NOT EAT ANY FOOD EXCESSIVELY.
* THE PATIENT SHOULD MOVE A LOT.
* FOODS THAT SHOULD NOT BE EATEN EXCESSIVELY:
– MILK AND MILK PRODUCTS
-SNACKS SUCH AS NUTS
– CHOCOLATE
– STRAWBERRY
– COLA DRINKS
– TEA – COFFEE
GENERAL MEDICAL EXAMINATION HAS THREE PURPOSES
To be able to find underlying metabolic and/or secondary causes.
To be able to find specific stress factors if any.
To determine current metabolic activity of the patient.
Stress factors:
Insufficient fluid intake ( less than 1 liter per day) – imbalance on diet (excessive irregular nutrition; for example, to eat meat only or to eat vegetable only) – immobilization – excessive absorbable alkaline Ca intake, excess Vitamin C, excess Vitamin D, CAH (carbonic anhydrase) inhibitors intake
In general, hyperparathyroidism, RTA (Renal Tubular Acidosis) and infection stones are common in women; and idiopathic uric acid and gout induced stones are common in men.
METABOLIC ASSESSMENT
Some test must be performed for the patients who state that they had passed stones more than one and it should be controlled that whether thet have any disease causing stone formation.
For those who have Ca stones;
Ca, Uric acid, oxalate, citrate, sodium, Mg, Phosphate, urine quantity and pH within the 24 hours urine; and Urea (BUN), Creatinine, Ca, PO4, Uric acid and Parathyroid Hormone (PTH) levels within the blood are analyzed.
The most common abnormality is hypercalcemia.
THERAPEUTIC OR PROTECTIVE AGENTS USED FOR PATIENTS WITH STONE
- Alkalinizing
K citrate:
It increases urine pH 0.7 to 0.8 pH unit. It is used as 60 mEq for 3 to 4 doses. K citrate increases excretion with 400 mg/d.
It is indicated for the patients who have Ca-oxalate stone secondary to hypocitratemia (<320 mg/d) and Renal Tubular Acidosis (RTA).
It may be used for the treatment of Uric acid stones and Ca-oxalate stones.
NAHCO3 and KHCO3 and orange juice are alternative alkalinizing drugs.
- Absorption Inhibitors Effective From Gastrointestinal System
Cellulose Phosphate:
It binds the intestinal Ca and reduced ca absorption from the intestines into the blood and Ca excretion within the urine accordingly. It is effective on Type 1 absorptive type Hypercalcemia with recurrent Ca stones. It prevents new stone formation. It reduces urinary saturation of ca oxalate and Ca phosphate in the urine. It should be taken 5 mg with meals.
Urinary Mg, Ca, Oxalate, sodium levels and PTH levels should be followed once or twice a year for follow-up. Mg supplementation is frequently necessary and it should be taken 1 hour before or after cellulose phosphate intake. Cellulose phosphate is together with Na( sodium) load and it should be used carefully when Chronic Heart failure is present.
It may cause dyspepsia and rarely diarrhea. Cellulose phosphate treatment on postmenopausal woman is sub-optimal. Citrate supplemented hydrocholorotiazids are giving by balancing potential hypoptassemia (reduction of potassium within the blood) and hypocitratemia.
Cellulose Phosphate: Should be used with Low Ca diet + Low oxalate diet + Low Na diet + Low Vitamin C + High Mag diet.
- Phosphate
It is used for renal phosphate loss. Antacids including aluminum, Mg and Ca reduces PO4 absorption.
- Diuretics
Thiazides reduce renal Ca loss in renal hypercalcemia. This prevents secondary Hyperparathyroidism. Thus, it reduces intestinal Ca absorption in combination. A rapid recovery is observed on renal Ca excretion and it is titrated according to the urinary Ca quantity. Hypopotassemia and serum hypocitratemia may occur and K may require to correct this.
- Drugs Reducing Uric Acid
Allopurinol which is used for the treatment of patients with stones and high uric acid level in the blood decreases Xantin oxidase and seum -urine uric acid levels. (serum idrar?) Allopurinol is a dangerous drug and it may be required to discontinue as soon as urticaria which may be fatal is observed. Treatment starts with 100mg/d and titration is performed according to urinary uric acid levels. It should be taken after meals.
- Urease inhibitors
Acetohyroxamic (AHA) acid which inhibits bacterial urease and reduces urinary NH4 and acidifying the urine accordingly may be used for struvite stones. Prophylactic use after removal of struvit stones results well. When serum Ca >2.5 mg/dl, sufficient urine level does not appear. It is ineffective on bacteria which do not produce urease. There is not any long term study. Side effects are frequent (headache, nausea, vomiting, anorexia, nervousness and depression). Dose: 250mg (3 to 4 times a day)
- Prophylaxis of Cystine Stones
Increase of fluid intake, alkalinizing the urine. Cystine solubility: When pH increases, cystine solubility increases. D-Penicillamine is not dissolved, reduces cystine quantity. Side Effects (skin lesions, hemathological, renal abnormalities). Dose: 250mg ( 2 to 3 doses) Max. 2 g. Pyridoxin should be given together.
Mercaptopropylenylglycin is tolerated better than Penicillamin. Cystine is bound to the sulphide part and form disulphide compound which is soluble in water. Alpha-MPG delays new stone formation. Dose: 200 to 300 mg 3 x/d 1 hour before or 2 hours after the meal.
Side Effects (fever, nausea-vomiting, loss on taste sense, hemathological diseases).
DRUGS USED FOR CHEMOLYSIS (STONE DISSOLVING) : Stone dissolving agents may be used by washing the inner side of the kidney though a percutaneous catheter which is left within the same session with PCNL in general or after. A careful utilization is required. It should be applied on hospital conditions.
Acidic solution : It may be used for STRUVITE stones.
RENACIDIN SOLUTION
SUBY’S G SOLUTION
Alkalinizing solutions: They may be used for uric acid or cystine stones.
NaHCO3 Solution
THAM- E or THAM-E + ACETYLCYSTEINE
STONE ANALYSIS METHODS
Analysis of the inner structure of the stone particles removed by open surgery or closed techniques is important to regulate further life conditions.
- CHEMICAL
- Qualitative: The most common method
- Quantitative
- Chromatographic
- MICROSCOPIC Crystal shape is analyzed
- INSTRUMENTAL
- Scanning electron microscopy
- Transmission electron microscopy
- Infrared microscopy
- Radiographic X-ray
- Spiral CT
- Spectrophotometric
METABOLIC CLASSIFICATION FOR UROLITHIASIS (urinary tract stones)
- IDIOPATHIC Ca Stones
Solute Excess
Hypercalciuric Ca nephrolithiasis (HCCNL)
(abrosptive-resoptive- renal Ca leak – renal phosphate leak)
Hyperoxaluric Ca nephrolithiasis (HOCNL)
Hyperuricosuria Ca nephrolithiasis (HUCNL)
Hypocitric aciduric conditions
Inhibitor deficiency
- URIC ACID STONES
Gout- myeloproliferative diseases – conditions where urine volume decreases
- HYPERCALCEMIC CONDITIONS
Primary Hyperparathyroidism- immobilization- sarcoidosis- hypercortisonism- hyperthyroidism- hyper Vitamin D- Malignencies- Milk Alkaline Syndrome
- INTESTINAL MALABSORPTION
Enteric hypercalciuria – uric acid
- RENAL TUBULAR SYNDROMES
RTA (renal tubular acidosis) – Cystinuria
- ENZYMATIC DISEASES
Xantinuria- primary hyperoxaluria
TREATMENT PRINCIPLES FOR Ca STONES ACCORDING TO THEIR ETIOLOGIES
* EXCESSIVE FLUID INTAKE + Na AND OXALATE RESTRICTION IN THE DIET
* Ca RESTRICTION IN THE DIET
(it is contraindicated in renal hypercalciuria (it should not be done))
ABSORPTIVE HYPERCALCIURIA TYPE 1
Na Cellulose phpsphate + Mg citrate + Hydrocholortiazide + K Citrate
ABSORPTIVE HYPERCALCIURIA TYPE II
Decrease the Ca within the diet (400 mg/day)
RENAL HYPERCALCIURIA
Hydrocholorthiazide + K Citrate
PHOSPHATE LEAK
Orthophosphates